Arthritis of the Wrist & Hand
Inflammation and joint wear affecting the wrist and hand
Arthritis is a condition that causes inflammation and gradual wear of the joints. When it affects the wrist and hand, it can lead to pain, stiffness, swelling, and reduced grip strength. Everyday activities such as turning a key, opening jars, typing, or lifting objects may become more difficult as the condition progresses.
There are several different types of arthritis that can involve the wrist and hand, including osteoarthritis (age- or wear-related changes), rheumatoid arthritis (an autoimmune condition), and post-traumatic arthritis (following an injury such as a fracture or ligament damage).
Diagnosis and treatment are tailored to the specific type of arthritis and the impact it is having on your daily life. Options may range from non-surgical measures such as splints, medication, and hand therapy to surgical procedures when symptoms are more advanced.
Prof .Vera Sallen will work with you to identify the cause of your symptoms and guide you through the treatment options most suitable for your needs and lifestyle.
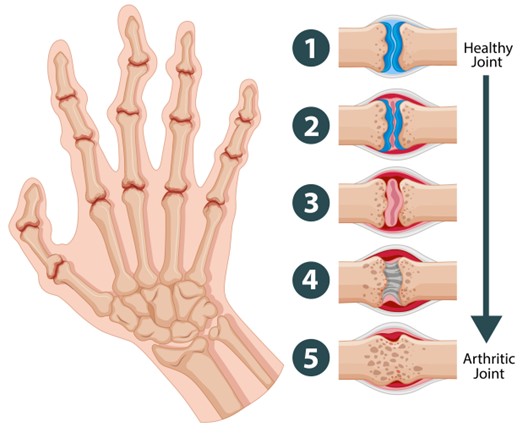
Causes of Arthritis of the Wrist & Hand
Arthritis in the hand develops when the smooth cartilage that lines the small joints begins to break down. Cartilage normally acts as a cushion, allowing your joints to move smoothly. When it wears away, the bones rub against each other, leading to pain, swelling, and stiffness.
Several different types of arthritis can affect the hand, each with its own underlying causes:
- Osteoarthritis: A common type of arthritis that occurs when the cartilage in the hand joints wears down over time, leading to bone-on-bone friction.
- Rheumatoid Arthritis: An autoimmune disorder in which the body’s immune system attacks the joint linings, causing inflammation, pain, and potential joint deformities.
- Post-Traumatic Arthritis: Arthritis can develop in the hand following an injury, such as a fracture or ligament tear, as damaged joints are more prone to degeneration.
- Genetic Factors: Family history can play a role, as some people may inherit a predisposition to arthritis.
- Age and Overuse: Wear and tear from repetitive hand movements over time can contribute to joint degeneration.
Symptoms of Arthritis of the Wrist & Hand
Arthritis in the hand can cause a range of symptoms that may develop gradually or worsen over time. The specific joints affected and the type of arthritis play a role in how symptoms appear, but some common features include:
Pain and discomfort
- Aching or sharp pain in the joints of the fingers, thumb, or wrist.
- Pain may be worse with activity, such as gripping, pinching, or twisting.
- Some people experience pain even at rest or during the night.
Stiffness and reduced movement
- Difficulty bending or straightening the fingers or thumb fully.
- Stiffness often feels worse in the morning or after periods of inactivity.
- This can make daily tasks such as writing, opening jars, or turning keys more challenging.
Swelling and tenderness
- The joints may appear puffy, swollen, or tender to the touch.
- In rheumatoid arthritis, swelling may involve multiple joints on both hands.
Changes in joint shape
- Bony enlargements at the joints of the fingers (often seen in osteoarthritis).
- Deformities, such as drifting of the fingers, are more common in rheumatoid arthritis.
Weakness and loss of function
- Reduced grip strength and difficulty holding objects firmly.
- A feeling of instability at the base of the thumb, especially in advanced arthritis.
Other possible symptoms
- A grinding or clicking sensation (crepitus) when moving the joints.
- Warmth or redness over the affected joints in cases of inflammatory arthritis.
If you are experiencing these symptoms, Prof Sallen will carefully assess your hands to determine whether arthritis is the cause and discuss the most appropriate next steps in diagnosis and treatment.
Diagnosis of Arthritis of the Hand
Medical history
The first step in diagnosing arthritis is a detailed discussion of your symptoms. Prof Sallen will ask about the type of pain you are experiencing, when it occurs, and how it affects your daily activities. Information about past injuries, family history of arthritis, or other medical conditions such as autoimmune disease can also provide important insights.
Physical examination
A thorough clinical examination of your hands and wrists helps to identify signs of arthritis, such as:
- Tenderness and swelling around affected joints
- Restricted range of motion or stiffness
- Grip strength and hand function
- Visible changes in joint shape or alignment
Imaging tests
- X-rays are commonly used to confirm a diagnosis. They can show joint space narrowing, bone spurs, or other changes typical of arthritis.
- Ultrasound may be used to detect inflammation or early cartilage damage.
- MRI scans are not always required but can provide detailed information if symptoms are unclear or if early disease is suspected.
Laboratory tests
If inflammatory arthritis such as rheumatoid or psoriatic arthritis is suspected, blood tests may be arranged to look for specific markers of inflammation or autoimmune activity.
Establishing a diagnosis
In most cases, arthritis of the wrist and hand can be diagnosed through a combination of history, physical examination, and imaging. Prof Sallen will explain the findings clearly and discuss the next steps, which may include non-surgical or surgical treatment options depending on the severity of the condition and your individual needs.
Treatment Options for Arthritis of the Wrist & Hand
Treatment for arthritis in the wrist and hand is designed to reduce pain, maintain mobility, and improve daily function. The best approach depends on the type of arthritis, the joints involved, and how much the condition affects your activities.
Non-surgical management
Many people find their symptoms can be managed with non-surgical care, particularly in the early stages. Options may include:
- Activity modification – Adjusting or avoiding activities that worsen pain, such as repetitive gripping or heavy lifting.
- Splints or braces – Wearing a supportive splint can help rest the affected joints and reduce strain.
- Medications – Non-steroidal anti-inflammatory medicines (NSAIDs) may relieve pain and reduce inflammation.
- Injections – Corticosteroid injections into the affected joint may provide temporary relief in selected cases.
- Hand therapy – A physiotherapist or hand therapist can provide tailored exercises to improve mobility, strengthen supporting muscles, and offer ergonomic advice.
Surgical options
If non-surgical treatments are no longer effective and symptoms significantly limit your quality of life, surgery may be considered. The type of operation depends on which joints are affected and the severity of arthritis. Options may include:
- Joint debridement – Removing inflamed tissue or loose fragments from the joint to ease discomfort.
- Joint fusion (arthrodesis) – Fusing two bones together to remove painful motion and improve strength and stability.
- Joint replacement (arthroplasty) – In some cases, the damaged joint can be replaced with an artificial implant to restore movement and reduce pain, most commonly at the base of the thumb.
Recovery and long-term management
Recovery depends on the type of treatment. With non-surgical care, symptom improvement may be gradual and ongoing. After surgery, a period of immobilisation, hand therapy, and guided exercises is usually recommended to restore function. Long-term management often involves a combination of self-care, therapy, and, if needed, surgical intervention.
Prof. Sallen will discuss which treatment options best suit your condition, daily needs, and lifestyle goals, and guide you through each step of your care.