Cervical Spine Radiculopathy
Relieving nerve-related neck and arm pain caused by compression in the cervical spine
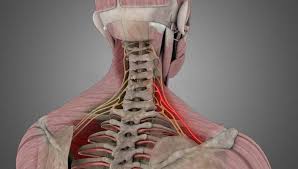
The cervical spine, or neck, supports the weight of your head, protects the spinal cord, and allows a wide range of movement. Cervical spine radiculopathy occurs when one of the nerves exiting the spinal cord in the neck becomes compressed or irritated. This may lead to pain, numbness, tingling, or weakness that can travel from your neck into your shoulder, arm, or hand.
This condition is commonly associated with age-related changes in the spine, such as disc degeneration or the development of bone spurs. It may also occur due to a disc herniation or following an injury. The way symptoms present can vary, and the most appropriate management approach will depend on the severity of your symptoms, any neurological changes, and the impact on your day-to-day function.
At Melbourne Orthopaedic Clinic, a structured assessment is used to understand the source of nerve irritation. This typically includes a detailed clinical examination and appropriate imaging, which helps guide treatment options tailored to your individual presentation.
- What is cervical spine radiculopathy?
- Common causes of cervical radiculopathy
- Symptoms of cervical radiculopathy
- How cervical radiculopathy is diagnosed
- Non-surgical treatment options for cervical radiculopathy
- Surgical treatment for cervical radiculopathy

What is cervical spine radiculopathy?
Cervical spine radiculopathy refers to irritation or compression of a nerve root as it exits the spinal cord in your neck. These nerves travel from the cervical spine into your shoulders, arms, and hands, playing an important role in movement, strength, and sensation.
When a nerve root becomes compressed or inflamed, it can disrupt normal nerve function. This may result in symptoms such as pain, altered sensation, or weakness that radiates from your neck into the upper limb. The pattern of symptoms often depends on which specific nerve is affected.
Each nerve root in the cervical spine corresponds to a particular area of the arm and hand. For example, some nerves are responsible for shoulder movement, while others contribute to hand and finger function. As a result, cervical radiculopathy can present differently from one person to another.
This condition is sometimes referred to as a “pinched nerve” in the neck. While this term is commonly used, cervical radiculopathy is a more accurate medical description of nerve irritation or compression within the cervical spine.
In many cases, cervical radiculopathy develops gradually over time due to changes within the spine. In other situations, it may occur more suddenly, particularly if related to a disc injury or acute strain.
Understanding the source and pattern of your symptoms is an important first step in guiding appropriate management.
Common causes of cervical radiculopathy
Cervical radiculopathy can develop when structures within the neck place pressure on, or irritate, one of the spinal nerve roots. This is most commonly related to changes in the spine that occur over time, although it can also result from more acute injury.
Some of the more common causes include:
Disc degeneration (wear and tear of the spine)
As part of the natural ageing process, the intervertebral discs can lose height and hydration. This may reduce the space available for the nerves and contribute to irritation or compression.
Bone spurs (osteophytes)
With ongoing degeneration, the body may form small bony growths around the joints of the spine. These bone spurs can narrow the pathways where nerves exit the spine, leading to pressure on the nerve root.
Disc herniation (bulging or prolapsed disc)
A cervical disc can bulge or rupture, allowing its inner material to press against a nearby nerve. This is a common cause of more sudden onset symptoms, particularly in younger or middle-aged individuals.
Foraminal stenosis (narrowing of the nerve exit space)
The foramina are small openings through which the nerve roots leave the spinal canal. Narrowing of these spaces, often due to a combination of disc changes and bone spurs, can compress the nerve.
Injury or trauma
Acute injuries such as falls, sporting incidents, or motor vehicle accidents may place sudden stress on the cervical spine, potentially leading to disc injury or inflammation around the nerve.
Less common causes
In some cases, cervical radiculopathy may be associated with other underlying conditions affecting the spine, such as inflammatory or structural disorders. These are less common but may be considered where symptoms or imaging findings are atypical.
Often, cervical radiculopathy is the result of a combination of these factors rather than a single cause. Identifying the underlying source of nerve compression is an important step in guiding appropriate treatment.
Symptoms of cervical radiculopathy
Cervical radiculopathy can cause a range of symptoms that typically extend beyond the neck and into the shoulder, arm, or hand. These symptoms occur when a nerve in the cervical spine is irritated or compressed, affecting how signals are transmitted between the brain and upper limb.
Symptoms may vary depending on which nerve root is involved, as each nerve supplies different areas of the arm and hand.
Common symptoms may include:
Neck and radiating arm pain
Pain often begins in the neck and travels down into the shoulder, arm, or hand. It may feel sharp, burning, or electric in nature, and can vary in intensity.
Numbness or altered sensation
You may notice reduced sensation, tingling, or a “pins and needles” feeling in certain parts of the arm or hand. The distribution of these symptoms often follows a specific nerve pattern.
Muscle weakness
Compression of a nerve can affect muscle function, leading to weakness in the shoulder, arm, or hand. This may make it more difficult to lift objects, grip, or perform fine motor tasks.
Changes in reflexes
In some cases, nerve involvement may alter normal reflexes in the arm. These changes are typically assessed during a clinical examination.
Symptoms affected by movement
Certain neck positions or movements may aggravate symptoms, particularly those that place additional pressure on the affected nerve.
For some people, symptoms develop gradually over time, while others may experience a more sudden onset. The severity can also vary, ranging from mild and intermittent discomfort to more persistent or limiting symptoms.
If symptoms are ongoing, worsening, or affecting your ability to perform daily activities, further assessment may be recommended to better understand the underlying cause.
How cervical radiculopathy is diagnosed
Diagnosing cervical radiculopathy involves understanding your symptoms, assessing how your nerves are functioning, and identifying the underlying cause of nerve irritation or compression.
Assessment typically begins with a detailed clinical history. This includes discussing the location and pattern of your pain, any numbness or weakness, how long symptoms have been present, and whether certain movements or activities make them better or worse.
A focused physical examination is then performed to assess your neck movement, strength, sensation, and reflexes in the arms. Specific clinical tests may be used to help reproduce symptoms and identify which nerve root may be affected.
Imaging studies are often used to further evaluate the cervical spine and confirm the diagnosis. These may include:
X-rays
X-rays can provide information about the alignment of the spine and may show signs of disc height loss or bone spur formation.
MRI (Magnetic Resonance Imaging)
MRI is commonly used to assess the soft tissues of the spine, including the intervertebral discs and nerves. It can help identify disc herniation, nerve compression, or narrowing of the spinal canal or foramina.
CT scan (Computed Tomography)
In some cases, a CT scan may be recommended to provide more detailed information about the bony structures of the spine.
Nerve conduction studies or EMG (if required)
These tests may be used in selected cases to assess how well the nerves are functioning and to help differentiate cervical radiculopathy from other nerve-related conditions.
Not all patients will require every investigation. The choice of imaging or additional tests will depend on your symptoms, clinical findings, and how the condition is progressing.
A clear diagnosis helps guide appropriate management and ensures that treatment is tailored to your individual presentation.
Non-surgical treatment options for cervical radiculopathy
In many cases, cervical radiculopathy may be managed without surgery. Non-surgical treatment is often recommended as a first step, particularly when symptoms are mild to moderate and there are no significant neurological concerns.
The aim of treatment is to reduce nerve irritation, improve movement, and support your return to everyday activities.
Common non-surgical treatment options may include:
Activity modification
Adjusting certain movements or positions that aggravate your symptoms can help reduce strain on the affected nerve. This may include modifying work tasks, posture, or recreational activities.
Pain management strategies
Simple pain relief medications or anti-inflammatory medications may be recommended to help manage discomfort. These should be used under the guidance of your GP or treating practitioner.
Physiotherapy
A structured physiotherapy program may help improve neck mobility, strengthen supporting muscles, and reduce pressure on the affected nerve. Treatment may also include education around posture and movement patterns to support recovery.
Exercise and rehabilitation
Targeted exercises can play an important role in restoring function and reducing symptoms over time. These are usually progressed gradually based on your response to treatment.
Cervical traction (in selected cases)
Traction techniques may be used by a physiotherapist to gently reduce pressure on the nerve by creating space within the cervical spine.
Image-guided injections (if appropriate)
In some cases, a corticosteroid injection around the affected nerve may be considered to help reduce inflammation and provide temporary symptom relief. This can also assist in confirming the source of pain.
Non-surgical treatment may lead to improvement in symptoms over time, although the rate of recovery can vary between individuals. Ongoing review is important to monitor progress and determine whether further intervention may be required.
If symptoms persist, worsen, or significantly impact your quality of life, surgical options may be discussed as part of your overall management plan.
Surgical treatment for cervical radiculopathy
Surgical treatment may be considered when symptoms of cervical radiculopathy persist despite appropriate non-surgical management, or when there is significant nerve compression leading to progressive weakness, ongoing pain, or functional limitation.
The aim of surgery is to relieve pressure on the affected nerve and improve nerve function. The most appropriate procedure will depend on the underlying cause of compression, the location of the affected nerve, and your individual clinical presentation.
Common surgical procedures may include:
Anterior cervical discectomy and fusion (ACDF)
This is one of the most commonly performed procedures for cervical radiculopathy. It involves removing the affected disc from the front of the neck to relieve pressure on the nerve. The space is then stabilised using a bone graft or implant, allowing the vertebrae to fuse over time.
Cervical disc replacement (artificial disc surgery)
In selected patients, the damaged disc may be replaced with an artificial disc rather than fused. This approach aims to maintain motion at that level of the spine while relieving nerve compression.
Posterior cervical foraminotomy
This procedure is performed from the back of the neck and involves removing a small portion of bone or disc material to widen the space where the nerve exits the spine. It may be suitable in cases where compression is located more laterally.
The choice of procedure will depend on a number of factors, including the specific anatomy of the compression, the number of levels involved, and your overall spinal health.
As with any surgical procedure, there are potential risks and complications. These may include infection, bleeding, nerve injury, or ongoing symptoms. During your consultation, the potential benefits, risks, and expected recovery will be discussed in detail to support informed decision-making.
Recovery following surgery varies depending on the procedure performed and your individual circumstances. A structured rehabilitation plan, often involving physiotherapy, is typically recommended to support your return to daily activities.